Hello to all the Ordinary Decent Reader(s) out there. It’s National Pathology Week! Are you all excited for some pathology-related fun?! Or are you curious about what happens after you die? Think that’s morbid? Well, I spent the past month working in a mortuary so here goes my attempt explaining a little bit about one of the (many) roles of a pathologist. I’ve brought Sarah along to help me on this one!
DISCLAIMER: If you are at all uneasy with the idea of post mortems, or graphic imagery, this might be one to avoid. Go and read one of my gaming posts instead, or look at some pictures of cats. Here’s one to get you started.

DISCLAIMER THE SECOND: I can only speak for the system in the United Kingdom, mainly Wales and Northern Ireland as I’ve had experience in these systems, and Sarah knows the English system.
Post mortem, meaning after death, or autopsy, to see for oneself. They amount to one in the same. The examination of bodies after death to determine cause of death. Have you ever been curious as to what it entails? Ever wondered who deals with this side of life (and death)? It’s a whole new world for me, but I’m here to provide insight into the valuable service provided by mortuary staff and pathologists every day.
Contrary to your deepest darkest imaginings, it’s an incredibly clean and bright place. Three stainless steel tables in a spacious, minimalist room. Stainless steel surfaces. Whiteboards with organ weights recorded. Sinks and hoses. One could be mistaken for thinking it was a basic operating theatre, and in a way, that’s not a million miles from the truth. But the surgery performed here is too late to be of benefit to the dead. It is for the benefit of the living. To reveal the secrets held by the dead. To bring closure for families. Be it natural or unnatural death, accidental or criminal, valuable information can be gleamed from autopsy. The tools: the scalpel and the PM40.

Guess who died?
Believe it or not, death happens all the time. There were 607,172 deaths in the United Kingdom in 2017 (source: ONS, NRS, NISRA). Compared to most statistics, this one is pretty concrete. I didn’t say “over six hundred thousand”, because I can give the exact number. How can I do that? Every death requires certification. And death certification requires a cause of death, be it natural or otherwise.
As you would imagine, many deaths are the result of a preceding illness. There are, of course, accidental deaths, but these are in the minority. What if somebody dies and their doctor doesn’t know the cause of death? That’s where the Coroner comes in.

The Coroner investigates death. That’s their role, and one of their most powerful tools is the post mortem. If someone dies in the community unexpectedly, and an obvious cause cannot be identified, the Coroner may request a post mortem examination to determine the cause of death. It’s often difficult to determine the exact cause, but based on the post mortem findings, the most likely cause of death is decided. Or not. It may be that no cause of death is determined, even after additional tests. This is a less common scenario but arises from time to time, and the cause is recorded as unascertained.
Unexpected deaths in the community and deaths of cause unknown are just part of the Coroner’s workload. They also investigate suicide, and accident and misadventure. We are going to focus on hospital post mortems as murder is the preserve of Forensic Pathologists.
Enter the Mortuary
What seems like the most unnatural of processes is part of day to day life in the mortuary. The APTs (Anatomical Pathology Technicians/Technologists) perform evisceration of bodies on a daily basis, with Histo- and Forensic Pathologists carrying out the external examination and organ dissection.
The first step is identification. Before the body is brought to the mortuary, someone should have identified the patient and recorded this information on tags attached to the body and the accompanying paperwork. Along with an APT, the pathologist confirms the identity of the body. If there is any doubt or conflict regarding the identity this is resolved first before proceeding. You can imagine it’s pretty crucial to have the right body.

Next, the External Examination
The approach varies from pathologist to pathologist, but generally it encompasses a head to toe examination noting identifying features including hair and eye colour, tattoos, injuries, scars, the presence of medical devices, and anything that would point towards an unnatural cause of death. If there is a suspicion of foul play, say unexpected ligature marks or a surprise knife in the back, then the post mortem is stopped (if it’s being carried out by a histopathologist) and turned over to Forensic Pathology, who carry out a more thorough assessment and collect samples for DNA and fibre analysis. This is not required for the majority of post mortems ordered by the Coroner.
The next step is evisceration – removing the internal organs for closer examination. This is performed by APTs or trainee pathologists, and can take a variety of forms. The common approaches I have experience with include the “Y” incision with neck dissection, and the midline incision. The neck dissection involves separating out the layers of muscle in the neck and checking for evidence of bruising or bleeding on the muscle.

The tongue is then freed and removed, along with the windpipe (larynx) and gullet (oesophagus). The initial incision is extended down the midline, along the chest wall and abdomen wall to the pubic bone. The skin and muscle is reflected from the chest wall and abdomen, and the ribcage can then be assessed. Rib fractures resulting from CPR are common, and can be anterior or lateral. Good CPR tends to break ribs, but when the difference is between being alive with broken ribs and being dead with pristine ones, I know which I’d choose.
The ribcage is cut on both sides with rib shears, and removed along with the breastbone (sternum), revealing the pericardial sac containing the heart, and the two lungs. Next, the bowel is tied off and removed, checking for any tumours or obvious signs of infection or tissue death. Damage to the bowel wall generally causes fluid to collect in the abdomen, and death results from infection of the lining of the abdomen called peritonitis. The pelvic organs are also freed and removed for later examination.
The block with the tongue, heart, lungs, liver, stomach, pancreas and spleen can be removed in one go, and set aside for examination. If no obvious cause of death is found or the history is suggestive of a brain injury, the APTs will open the skull and remove the brain for closer examination. The presence of bleeding would suggest a brain haemorrhage, resulting from trauma or a ruptured aneurysm. Pus on the surface of the brain would point towards meningitis, which is an infection of the lining of the brain.
Once the evisceration is complete, the body cavity is examined for the presence of bleeding or injury. If required, the spinal cord or long bones can be removed and examined.
Time for the dissection. The organs are examined one by one, using a systematic approach. This varies, and different pathologists will dissect differently, but this is one potential method (Sarah would like to add she does dissection in a slightly different way as she uses a different evisceration technique).
The organ block is placed with the heart and lungs down, showing the aorta at the back. The aorta is the main artery leaving the heart, and supplies oxygenated blood to most of the body. It is opened with scissors, along with the branches coming off it. Here we are looking for atherosclerosis or “furring up” of the wall, and aneurysm, which is a ballooning of the vessel wall. The ballooning of the wall also weakens it. The aorta is under tremendous pressure from the pumping action of the heart, so the combination of high pressure and a weakened vessel can be disastrous. A ruptured aortic aneurysm means death, unless you were in a hospital being operated on immediately. The rate of blood loss is immense.
Next the vena cava, the great vein, is opened and examined. Some kidney tumours can extend along the vein, and also cause blood clot formation. The adrenal glands are best known for producing the “fight or flight” hormone, adrenaline, and can be identified in the fat above the kidneys. They are examined for tumours or bleeding. The kidneys are then removed from their capsules and examined for scarring or tumours. The ureters, carrying urine from the kidney to the bladder, are opened and examined. The kidneys can be removed completely and weighed. We usually leave the ureter attached to the left kidney to differentiate left from right. They are then cut and opened like a book to examine for damage or tumour.
Kidneys done, now onto the tongue. The tongue is sliced width-wise several times and checked for bruising and bleeding. The presence of tongue biting could help identify a seizure death. Moving down the tongue, the oesophagus is opened to look for ulcers and tumours, then reflected back off the trachea. The thyroid gland can be examined at this point, noting any enlargement, and removed if required later. The vocal cords are inspected for swelling, bruising, bleeding and tumours. Swollen vocal cords is also known as laryngeal oedema, and can result from an allergic anaphylactic reaction.
Now the integrity of the hyoid, a small vampire like bone above the Adam’s apple (thyroid cartilage), is checked. Damage to the hyoid is unnatural, and can indicate a traumatic cause of death such as hanging or strangulation. Bruising or bleeding into the strap muscles of the neck is another sign of traumatic injury, be it accidental or deliberate.
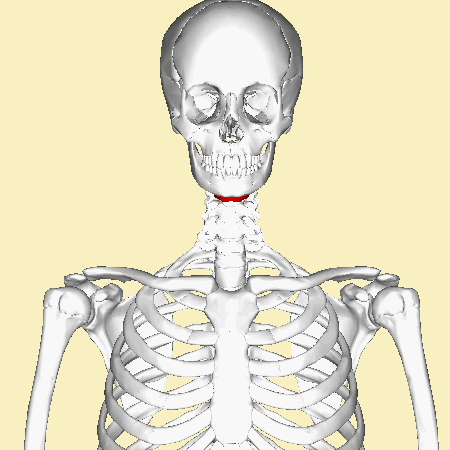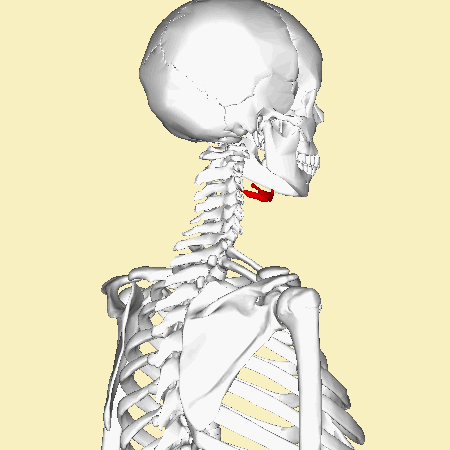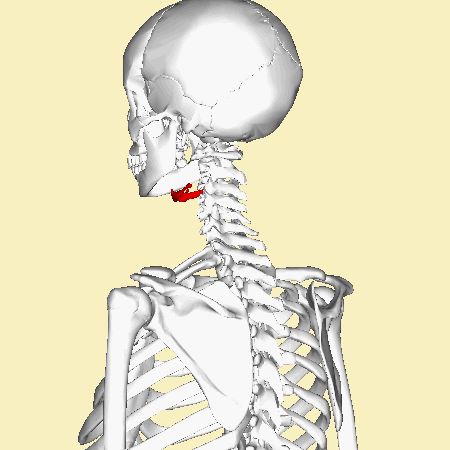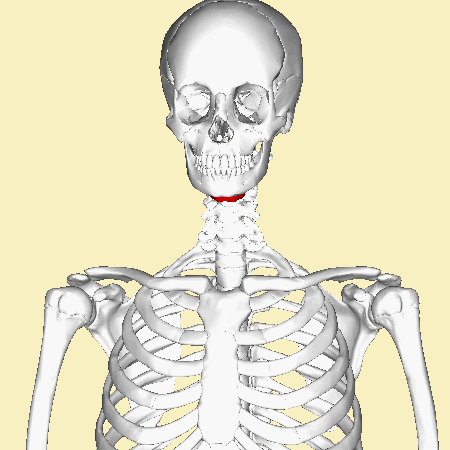
Time to open up the trachea and check for any excess mucus, or food that shouldn’t be there. Food in the lungs causes aspiration pneumonia – a rather nasty chest infection, which could be the cause of death.
The lungs are then removed and weighed, and examined for blood clots (pulmonary embolism), pus (infection), or fluid (pulmonary oedema). All of these interfere with the normal oxygenation of blood, and could kill you. The heart is enclosed within a bag called the pericardium, and it’s time to let the cat out of the bag. Just watch out for any blood, which could indicate a rupture of the heart muscle resulting from a heart attack, pus, or excess fluid (pericardial effusion). The heart is one of the most complex organs to dissect, and any abnormalities can kill you in a number of ways.
First, the origins of the coronary arteries are identified. These supply blood to the heart itself, and usually arise from the point the aorta leaves the left side of the heart. The three main coronary arteries are the left anterior descending, left circumflex, and right coronary artery. These are sliced in cross-section, and examined for narrowing (stenosis) or clot blocking the vessel completely (thrombosis). Blockage of a coronary artery leads to the muscle downstream becoming damaged, and eventually dying if the blood supply isn’t restored. This causes the classical “clutching chest and arm” pain that TV shows love. That’s where your friendly neighbourhood cardiologist comes in with his stent to re-open the blockage. Life is not always so kind as to give you enough time though, and damage to the heart can result in sudden death without warning.
We’re not finished with the heart quite yet, it still needs to be opened up. We slice off several sections from the base of the heart to examine for any fresh or old damage, then open the rest along the path the blood takes. From right atrium, to right ventricle and pulmonary artery (where the blood would normally travel to the lungs to be oxygenated). Then from left atrium, to left ventricle and finally out the aorta. The rest of the heart muscle is examined along with the valves, looking for any defects which could have resulted in or contributed to death. The heart is the only organ that is weighed after slicing, and a heavy or enlarged weight increases the risk of sudden death from a fatal rhythm disturbance.
Time for the stomach, which is opened from the oesophagus to the first part of the small intestine, the duodenum, and examined for ulcers, bleeding, or tumours. The main bile duct is also checked to ensure there is no blockage, and the gallbladder (if present) is checked for stones or signs of infection. The pancreas, the gland producing digestive enzymes and insulin and hiding behind the stomach, is examined for signs of bleeding, tumour, or old damage. The liver can be removed, inspected, weighed, and sliced to look for scarring, tumours, and changes related to disease elsewhere (such as heart failure).

The spleen, which has multiple functions including red blood cell recycling and storage and immune function, is inspected, weighed and sliced. It is one of the first organs to degrade after death, and can be almost liquid at post mortem.
Pelvic organs are up next. The rectum is opened and examined for tumours. For men, the prostate is opened into the bladder, and sliced to look for enlargement or cancer. The bladder is also examined for tumours or infection. In women, there is no prostate to contend with, but the cervix and uterus are opened to examine for cancer, followed by the Fallopian tubes and ovaries.
Finally, to the brain. The seat of consciousness. And one of the first organs to suffer degradation post mortem, along with the spleen and pancreas. It has been described post mortem as having the consistency of blancmange, and can be difficult to slice without distorting. We’re looking for any signs of bleeding, ischaemic stroke, or tumours.
If preservation of the structure is important or the brain requires more detailed examination by a neuropathologist, the brain is left unsliced and placed whole into a pot and covered with formalin. Formalin contains formaldehyde, which “fixes” the tissue, stopping decomposition and preserving the structure. It is also weighed, and the weight recorded on the trusty whiteboard.
And if we don’t find anything…
…then we fall back on our additional investigations.
Deaths due to alcohol or drugs can be difficult to determine from a straightforward post mortem, and often require additional toxicology tests. Blood and urine samples are collected and sent for analysis, and tissue samples can be taken and processed for microscopic examination. Pneumonia that may not be obvious on inspection of the lungs could be instantly recognisable under the microscope, along with damage from a heart attack.
And if we still don’t find anything
The death is unascertained. Sometimes we never find out what happened. It could have been a funny heart rhythm. An unexpected seizure. Another bizarre unknown condition. But these cases are in the minority, and often the cause of death will be related to heart dysfunction.
The findings are compiled into a report for the Coroner, which is then passed on to the family of the deceased. A proportion of cases will go to inquest at Coroner’s court, where the evidence will be reviewed and a determination of cause of death will be made.

That was a long one, but hopefully it gives you a little insight into what goes on in the mortuary, and the importance of the post mortem examination. As a little bonus for those of you that made it the whole way through – the mortuary I worked in was featured in the very first episode of Sherlock.

Leave a comment